Turn Reimbursement Risk Into Role-specific Action
From Insight to Intervention — Inside Real Workflows
RevProtect goes beyond identifying reimbursement risk. It prescribes specific, evidence-based actions to prevent denials and adverse payment outcomes. These recommendations are delivered directly within the workflows teams already use.

RevProtect Recommends
For each at-risk case, RevProtect provides clear guidance on:
RevProtect ensures claims are supported by the right evidence before submission, reducing the likelihood of adverse payment outcomes. When denials or downgrades do occur, teams already have the documentation needed to win disputes and appeals.
Built for real roles — not generic tasks
RevProtect identifies why reimbursement risk exists and delivers role-specific interventions.
Recommendations are grounded in denial type, DRG context, and payer behavior.
Every recommendation is tied to what each role can influence, reducing noise and increasing follow-through.
Role-specific action, by design
Clinical Documentation Improvement (CDI)
- Surface missing MCC/CC specificity
- Guide targeted provider queries tied to payer expectations
Utilization Review (UR)
- Flag level-of-care risk
- Recommend escalation to physician advisor when warranted
Coding
- Highlight modifier and duplication risk
- Identify coding edits likely to trigger payer review
Patient Financial Services (PFS) / Denials Teams
- Focus effort on high-probability overturns
- Surface the exact evidence needed to support appeals
How RevProtect Delivers Actionable Recommendations
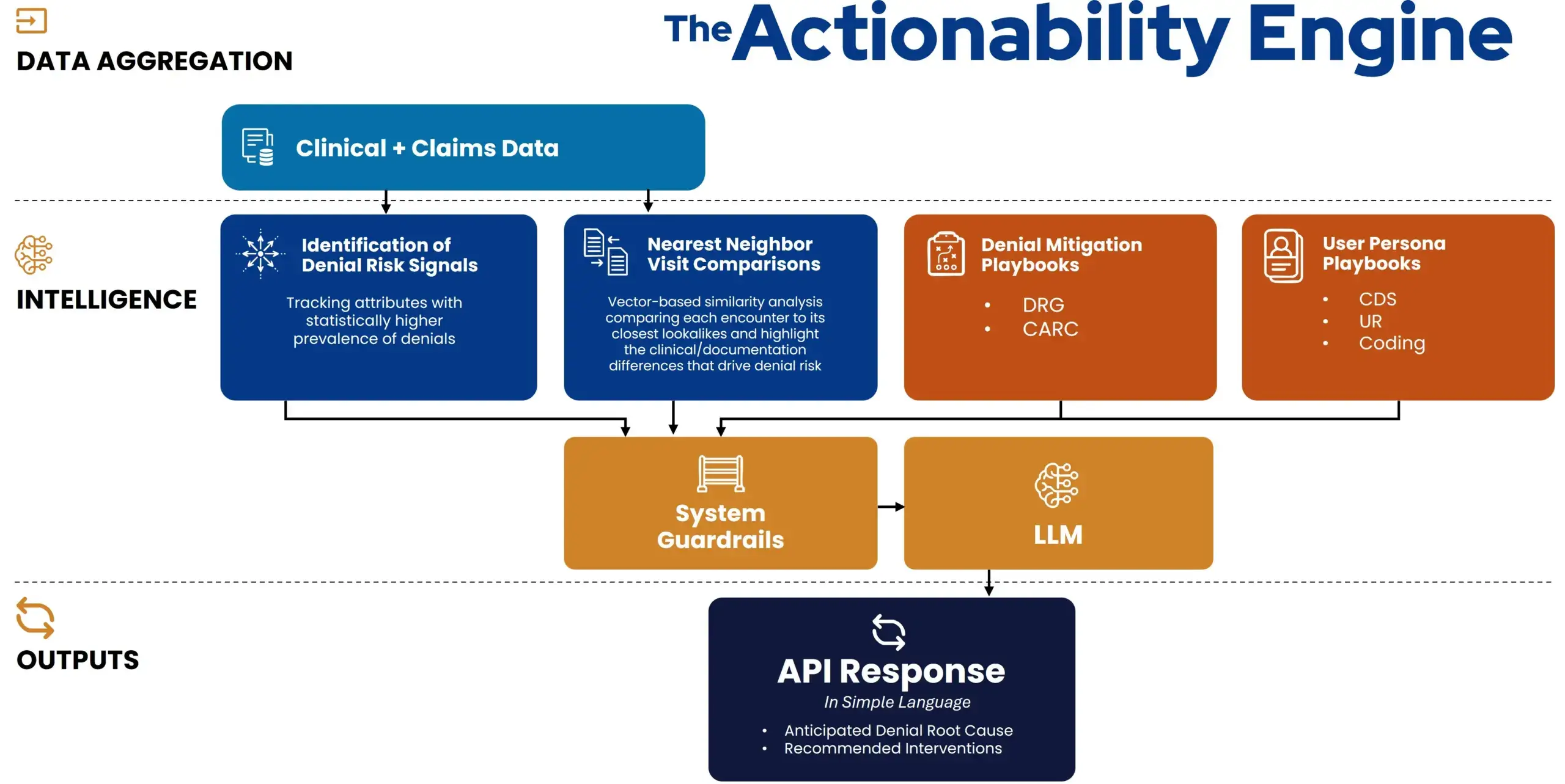
RevProtect combines multiple analytical layers to move from risk identification to action:
- Prediction layer surfaces reimbursement risk and root cause
- Look-alike modeling identifies statistically similar paid and denied cases
- Nearest-neighbor analysis highlights relevant clinical and documentation differences that matter
- Denial and persona playbooks translate risk into role-specific guidance
- System guardrails enforce confidence thresholds and escalation rules
- Plain-language outputs deliver clear actions and rationale via API or embedded workflows
This architecture ensures recommendations are precise, clear, and defensible.
Smarter with Every Outcome
As actions are taken and outcomes are realized, RevProtect continuously learns and adapts. This learning loop ensures the system improves with use, while maintaining governance and control.
Aligned to Outcomes, Not Promises
RevProtect is available through a performance-based engagement model designed to align incentives and reduce risk. Sift partners directly with health systems to tie success to measured reductions in denials and adverse payment outcomes (not activity, licenses, or usage).
Talk with us about whether a performance-based model makes sense for your organization.
