Post-Bill Recovery
Payer tactics are constantly changing. RevProtect helps revenue cycle teams recover more, faster, by prioritizing the work that actually moves cash.
- Faster Cash
- Fewer wasted touches
- Measurable ROI for existing staff
Denials Are Inevitable. Wasted Effort Is Not.
Denials now cost the average hospital ~3.3% of net patient revenue. For the average hospital, that’s nearly $5M walking out the door. And reworking them costs an additional ~$118 per hospital-based claim:
- Too many denials and downgrades to work with limited Patient Financial Services capacity
- No reliable way to know which denials are worth pursuing
- Poor visibility into when payer follow-up will actually change outcomes
- Limited insight into denial-driven cash impact
- Disconnected analytics across denials, work effort, and expected recoveries
RevProtect applies payer-specific intelligence and machine learning to optimize recovery when prevention isn’t enough, enabling health systems to understand which denials are worth working, when payers are most likely to respond and where staff effort will actually convert to cash.
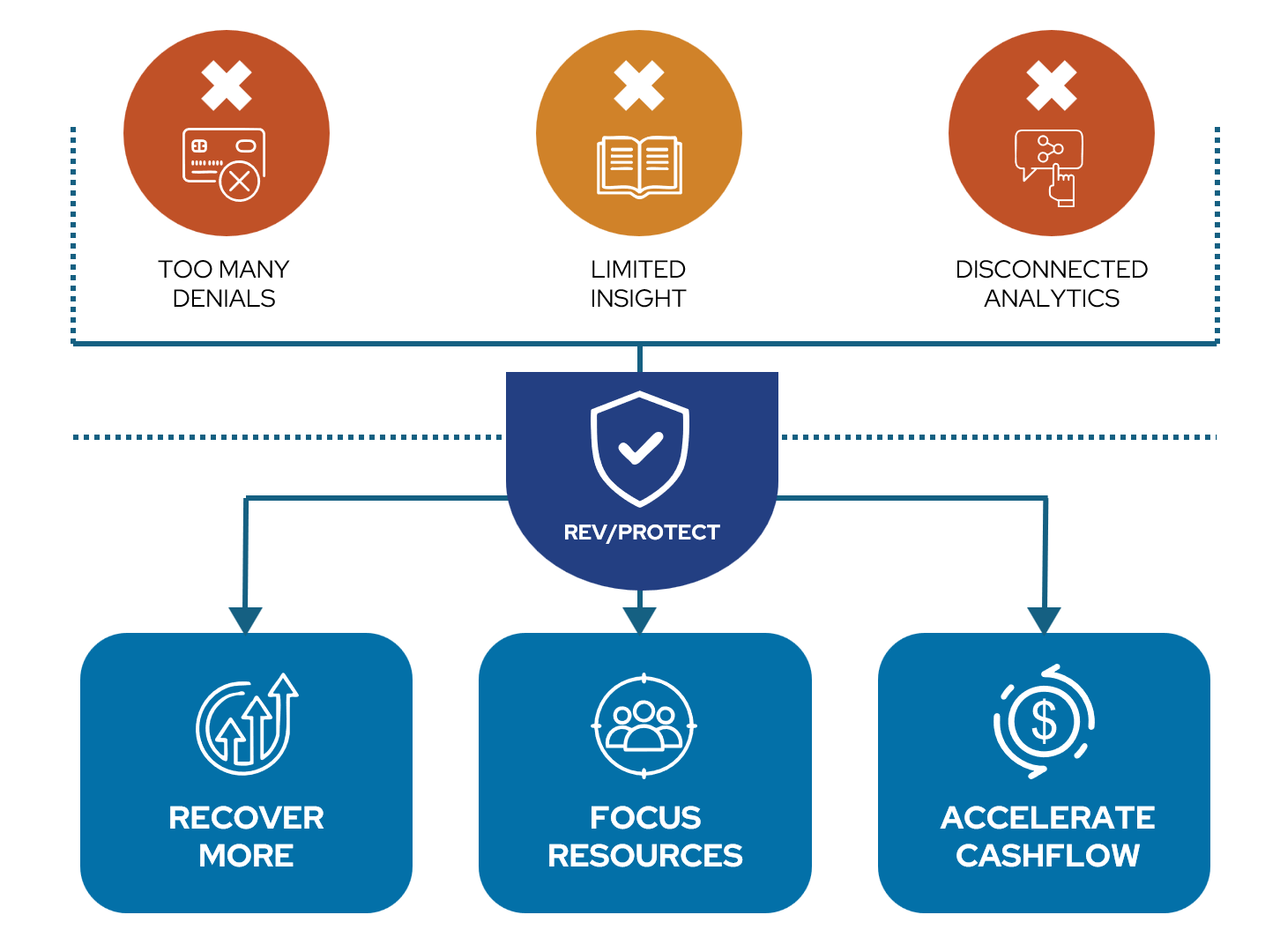
What RevProtect Optimizes After Submission:
RevProtect provides detailed visibility into reimbursement performance across the full denial and payment lifecycle.
By establishing a clear, data-driven view of payer behavior and reimbursement risk, health systems armed with RevProtect are equipped to proactively prevent adverse payment outcomes.
RevProtect intelligence powers:
- Adverse payment outcome predictions
- Actionable recommendations that guide prevention and recovery
- Validation and learning that measures impact and continuously improves performance
Do More With the Team You Have
RevProtect helps revenue cycle leaders:
- Reduce low-value touches
- Shorten time-to-cash
- Increase recovery rates without adding headcount
- Tie daily work directly to financial outcomes
Talk with us about how revenue recovery intelligence fits into your RevProtect strategy.
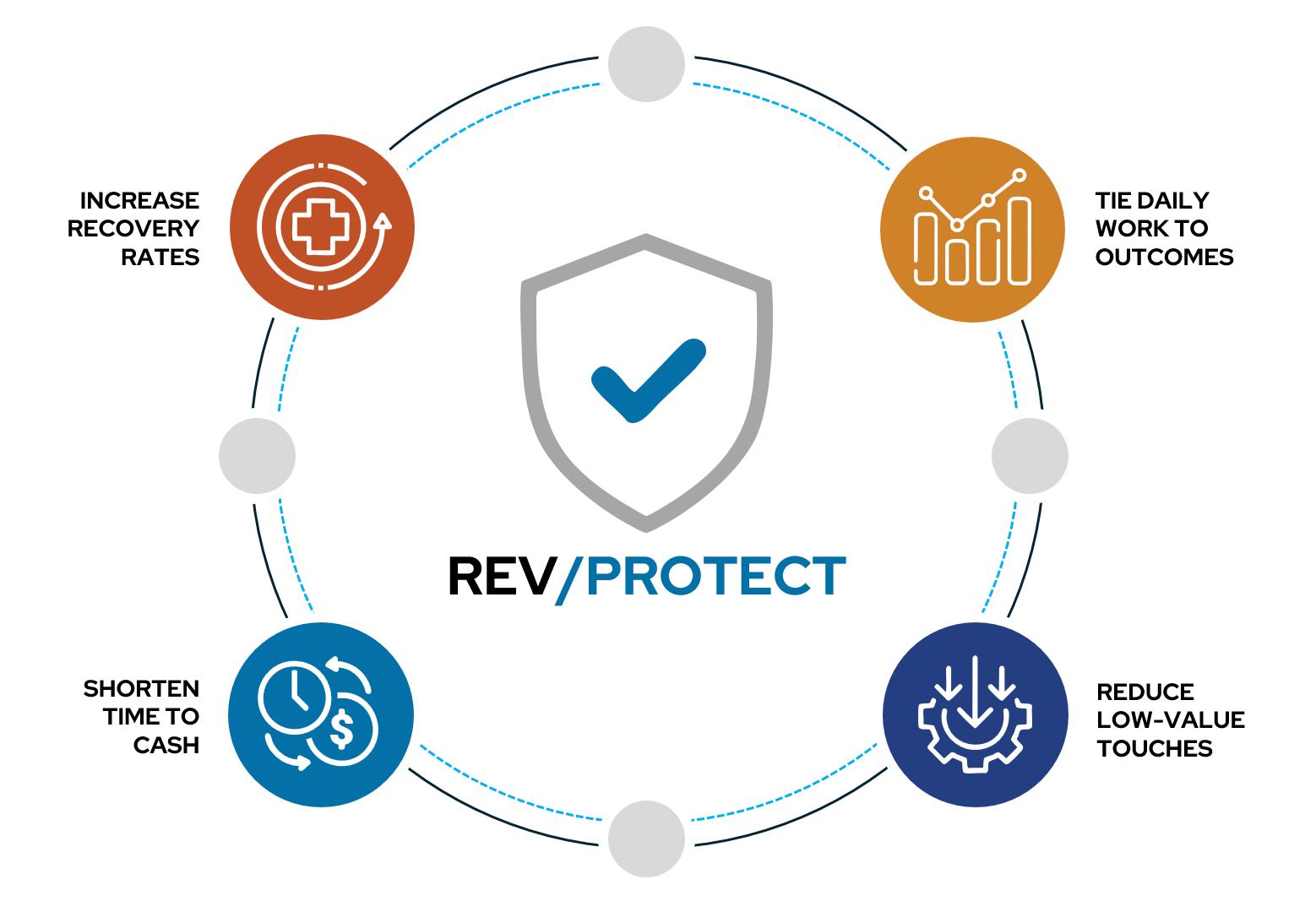
Aligned to Outcomes, Not Promises
RevProtect is available through a performance-based engagement model designed to align incentives and reduce risk. Sift partners directly with health systems to tie success to measured reductions in denials and adverse payment outcomes (not activity, licenses, or usage).
Talk with us about whether a performance-based model makes sense for your organization.
