Prove Impact. Improve Performance. Repeat.
Revenue cycle teams need more than anecdotal wins. They need proof that interventions are working and a system that gets smarter over time.
Close the Loop Between Action and Outcomes
RevProtect provides the validation and learning layer that turns prediction and action into measurable, repeatable financial impact.
Through real-time performance monitoring and continuous learning, health systems can track reimbursement risk over time, measure the effectiveness of interventions, and continuously refine revenue protection strategies with confidence.
Measure What Works
RevProtect delivers comprehensive dashboards and reporting that give leaders clear visibility into how reimbursement risk and outcomes change over time.
Health systems can track performance across:
These insights allow teams to move beyond anecdotal wins and clearly demonstrate where revenue protection efforts are working and where adjustments are needed.
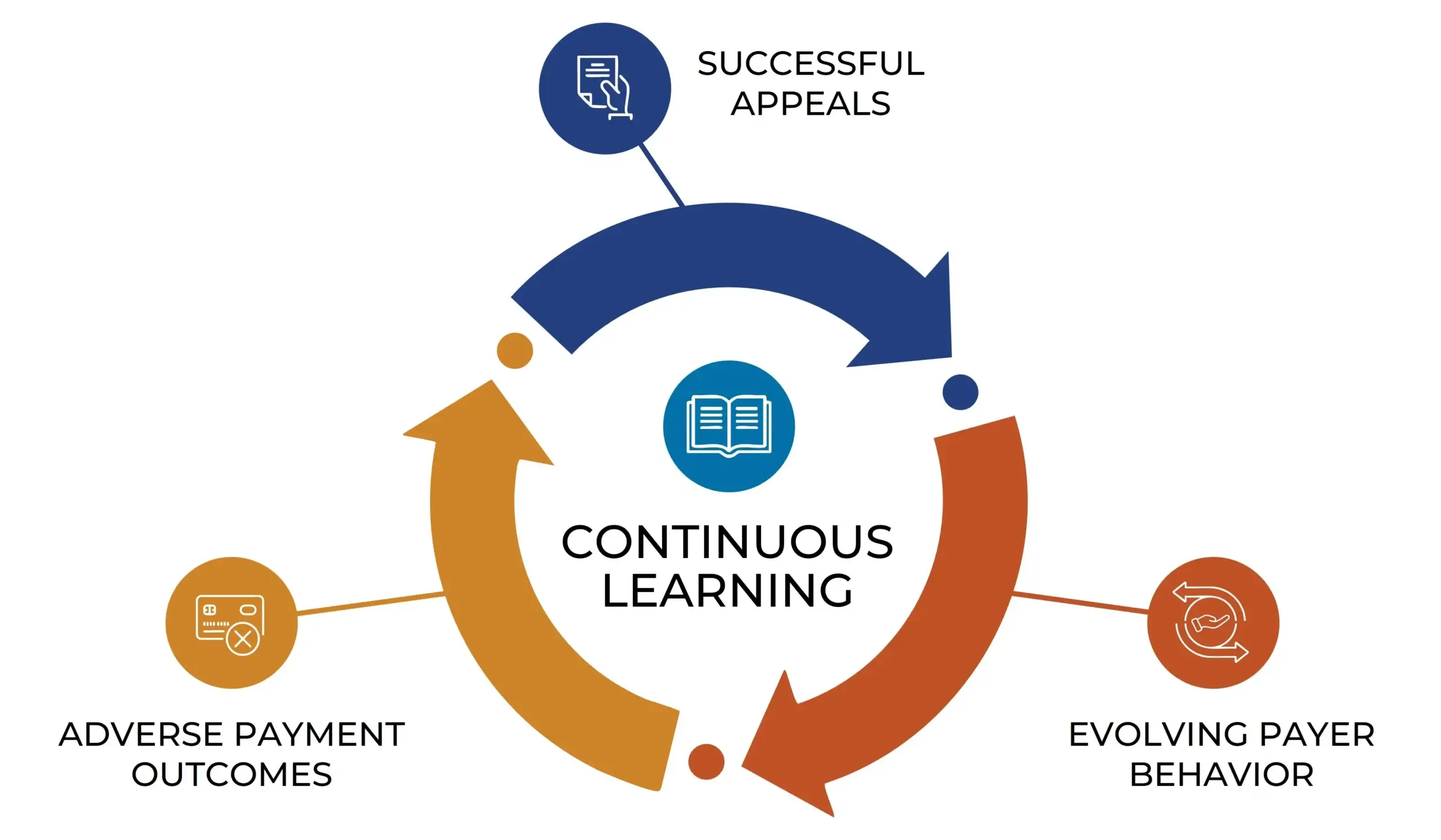
Get Smarter With Every Claim
Every outcome strengthens RevProtect’s performance:
- Adverse payment outcomes provide new training data on payer-specific risk patterns
- Successful interventions and appeals inform future recommendations
- Changes in payer adjudication behavior are detected and incorporated
- Model accuracy improves over time as more payment outcomes are observed
- Provider-specific patterns enable tailored risk scoring
This feedback loop ensures RevProtect adapts to changing payer requirements, regulatory shifts, and organizational workflows.
Built for Long-term ROI
RevProtect’s validation, insights, and reporting equip health systems with:
- Confidence that recommendations are working – Track intervention effectiveness in real time
- Transparency into ROI and time-to-cash impact – Measure financial outcomes at the case and portfolio level
- A governed path to automation and deeper workflow integration – Scale what works with control and visibility
RevProtect is an intelligent system that learns from every clinical, claim, and payment data point, continuously sharpening its prediction and prevention accuracy.
Aligned to Outcomes, Not Promises
RevProtect is available through a performance-based engagement model designed to align incentives and reduce risk. Sift partners directly with health systems to tie success to measured reductions in denials and adverse payment outcomes (not activity, licenses, or usage).
Talk with us about whether a performance-based model makes sense for your organization.
